
Perianal Crohn's Disease
Treatment, causes, symptoms, diagnosis

 |
Perianal Crohn's Disease Treatment, causes, symptoms, diagnosis |
 |
|
| www.WhatsCrohnsDisease.com is written by real health professionals |
|---|
Web Pages on WhatsCrohnsDisease.com
The professionals behind WhatsCrohnsDisease.com
|
and Please share us with your online friends.
What is Perianal Crohn's Disease?Perianal Crohn's disease is characterized by skin lesions such as anal skin tags, anal abscess, as well as anal canal lesions such as perianal abscesses, fistulas, and fissures - all these symptoms of perianal Crohn's disease and colitis is fully described below. Perianal disease is more common in patients with colitis and ileocolitis than in small-bowel disease. In one-third of individuals, perianal disease precedes the onset of symptomatic intestinal disease. In other words, perianal afflictions often come before Crohn's disease or ulcerative colitis is present. The original description of Crohn's disease did not describe perianal lesions. It wasn't until 1938 that Penner and Crohn described the presence of a perianal fistula in a patient with Crohn's disease. There is strong evidence for a genetic contribution to perianal Crohn's disease. That perianal disease is a distinct type of Crohn's disease is supported by the recent identification of a susceptibility locus on chromosome 5. 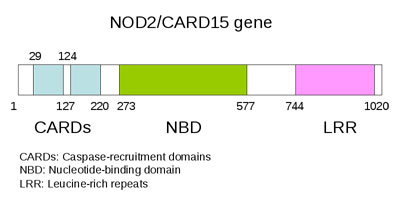
Above is a diagram of a gene believed to be responsible for Crohn's disease. Picture courtesy of Samir.
How Common Is Perianal Crohn's Disease?Perianal disease is a common complication of Crohn's disease in children and adolescents, females and males. Of 325 Crohn's patients, 200 (62%) developed perianal disease. i In 64 to 68 percent of patients with Crohn's disease perianal complication occurs at the same time or after the diagnosis of intestinal disease. Williams reported that 74 percent of these patients develop perianal lesions within 10 years of diagnosis of intestinal disease. The more distal the bowel involvement, the greater the prevalence of perianal disease. Thus, perianal disease is more common in patients with colitis and ileocolitis than in small-bowel disease. This was reported by Bergstrand et al who found that 92 percent of patients with rectal disease developed perianal fistula. Crohn's disease shows a peak incidence in females during their reproductive years. Thus, a high percentage will have active or new onset perianal disease during pregnancy. Perianal disease is usually an indication for caesarean section.
What Are the Symptoms of Perianal Crohn's Disease?Perianal discomfort is a sign of perianal Crohn's disease. Itchiness or pain around the anus, the external opening of the rectum, may be suggestive of inflammation, fistulization or abscess around the anal area or anal fissure. The severity of perianal Crohn's disease depends on the severity of the nonperianal disease. In other words, generally, the worse the diarrhea, the more symptomatic the perianal disease. In a series of 356 Crohn's disease patients, Galandiuk et al. noted that more than 1 perianal fistula was the most common type of perianal disease (87%).ii This was followed in frequency by fissure (44%) and anal-canal stricture (37%). In another study of patients with perianal Crohn's disease, anal skin tags were present in 35% of patients, fissures in 51%, fistulas in 15%, and abscesses in 13%.iii Anal AbscessAn abscess is a pocket of pus near the intestine caused by infection from bacteria. This pocket of infection requires drainage either through a catheter inserted by a radiologist or a special drain that is surgically inserted. An abscess causes tenderness, swelling, and pain. These symptoms disappear when the abscess is drained. Individuals may also complain of fever, chills, and general weakness or fatigue. Whenever the physician finds an abscess, and especially a fistula, further tests are needed to be sure Crohn's disease is not present. Anal abscess is present in 13% of Crohn's patients.iv Anal Fissure
Anal fissure is present in approximately 51% of patients with Crohn's disease.v An abscess or fistula can subsequently develop in 26 percent of individuals with a fissure. Anal FistulasAnal fistulas are most common in people with Crohn's disease.vi In Crohn's disease sores or ulcers develop within the intestinal tract. Sometimes these deep ulcers turn into tracts / tunnels—called fistulas—that connect via the hole different parts of the intestine. But fistulas may also tunnel into surrounding tissues such as the bladder, vagina, or skin around the anus (Figure 2, right). These holes typically spread the infection that creates them, and life-threatening conditions such as peritonitis (inflammation of the lining of the abdomen) may occur. Anal fistulas develop in the presence of inflammation and infection and often drain pus or liquid which can soil or stain clothing (Figure 2, left). Often a draining fistula is not painful but it can irritate the skin around it. Fistulas can be internal, external, or mixed; single of multiple. If the fistula is small, antibiotics may be sufficient to heal it. Large or multiple fistulas, on the other hand, may signal the need for surgery, particularly if they are accompanied by fairly persistent symptoms, such as fever or abdominal pain. Often a fistula forms an abscess near the intestine which requires drainage. This can be done with a seton – a length of suture material looped through the fistula which keeps it open and allows pus to drain out. Usually when an individual presents with a fistula, flexible sigmoidoscopic examination is warranted to evaluate the mucosa of the distal colon for signs of Crohn's disease. The index of suspicion for Crohn's disease is increased by a history of episodes of diarrhea, abdominal cramping, weight loss, and the appearance, location and multiplicity of fistulas. Anal Skin Tags and HemorrhoidsAnal skin tags, also called Crohn's skin tags, frequently occur in Crohn's disease while hemorrhoids occur infrequently; only 0.04 percent of 20 patients with hemorrhoids were noted to have Crohn's disease over a 41 year period.vii
Anal skin tags have been classified into 2 types:
Anal skin tags are more commonly found in association with Crohn's disease (75.4%) compared to patients with ulcerative colitis (24.6%) and are more common in the presence of disease limited to the colon as compared to disease elsewhere in the bowel.viii Anal skin tags are diagnostic of Crohn's disease especially in young people with diarrhea, abdominal pain, and/or growth retardation. Anal skin tags are generally asymptomatic and often are the remnants of previously thrombosed external hemorrhoids. When tags are symptomatic, as a result of itching or hygienic problems, they can be removed. Local anesthetic is injected and the area is excised and then sutured or left to heal. But remember that any surgery below the dentate line causes considerable postoperative pain. Moreover, in patients with Crohn's disease, conservative management is advised because of the post-operative risk of poor wound healing, anorectal stenosis and the potential need for subsequent proctectomy.
Other Symptoms of Perianal Crohn's DiseasePerianal Crohn's disease can be extremely debilitating. Fecal incontinence may accompany perianal Crohn's disease. Perianal pain and fecal soiling greatly diminish an individual's quality of life. Perianal involvement can lead to social isolation because individuals have urgency, frequency, stool incontinence that can be related to either the disease itself of other complications. At the other end of the gastrointestinal tract, the mouth may be affected by non-healing sores called aphthous ulcers. The stomach and esophagus are rarely involved in Crohn's disease. However, if they are, this can cause difficulty swallowing, upper abdominal pain, and vomiting. Other symptoms include pain, soiling, sleep disruption, sexual dysfunction, and sepsis.
How is Perianal Crohn's Disease Diagnosed?The diagnosis of perianal Crohn's disease necessitates radiological imaging of the gastrointestinal tract. Most radiologists perform magnetic resonance imaging (MRI) under anesthesia which is particularly useful in the identification of undiagnosed fistula and in monitoring the effects of treatment. There are a number of questionnaires that are used to determine a patient's quality of life with perianal disease.
Does Perianal Crohn's Disease Cause Cancer?Perianal disease is associated with colorectal cancer. There is an increased risk of developing colorectal cancer in patients with perianal Crohn's disease.ix The earlier in your life that you develop Crohn's disease, the greater your risk for developing perianal complications and the greater your risk for developing colorectal cancer. Also known as fistula-related cancer, many people with Crohn's disease are surprised to learn that the condition is present after self-treating hemorrhoids during a flare-up. Adenocarcinoma mandates proctectomy (removal of the colon). Squamous carcinoma may be considered for chemo-radiotherapy although proctectomy is usually the preferred option.
References for Perianal Crohn's Diseasei Tolia V. Perianal Crohn's disease in children and adolescents. Am J Gastroenterol 1996; 91: 922-926.
ii Galandiuk S, Kimberling J, Al-Mishlab, Stromberg AJ. Perianal Crohn disease: Predictors of need for permanent diversion. Annals of Surgery 2005; 241: 796-802. iii Palder SB, Shandling B, Bilik R, Griffiths AM, Sherman P. Perianal complications of pediatric Crohn's disease. J Pediatr Surg 1991; 26: 513-515.
iv Palder SB, Shandling B, Bilik R, Griffiths AM, Sherman P. Perianal complications of pediatric Crohn's disease. J Pediatr Surg 1991; 26: 513-515.
v Palder SB, Shandling B, Bilik R, Griffiths AM, Sherman P. Perianal complications of pediatric Crohn's disease. J Pediatr Surg 1991; 26: 513-515.
vi Galandiuk S, Kimberling J, Al-Mishlab, Stromberg AJ. Perianal Crohn disease: Predictors of need for permanent diversion. Annals of Surgery 2005; 241: 796-802. vii Jeffery PJ, Parks AG, Ritchie JK. Treatment of hemorrhoids is patients with inflammatory bowel disease. Lancet 1977; 1: 1084-1085. viiiBonheur JL, Braunstein J, Korelitz BI, Panagopoulos G. Anal skin tags in inflammatory bowel disease: New observations and a clinical review. Inflamm Bowel Dis 2008; 14: 1236-1239.
ix Sjodahl RI, Myrelid P, Soderholm JD. Anal and rectal cancer in Crohn's disease. Colorectal Dis 2003; 5: 490-495. x Basu A, Wexner SD. Perianal Crohn's disease. Lancet 1975; 1: 775-777.
Written by Dr. Kirchgessner, edited by Donald Urquhart This is an educational web site. It is NOT designed to diagnose nor treat but to offer understanding, ideas and options for you to discuss with your doctor first. Also, please consider adding our site to your bookmarks or favorites and sharing us with your online friends. Our Privacy Policy can be found at www.cholesterolcholestrol.com/privacypolicy.htm Copyright © 2000-present Donald Urquhart. All Rights Reserved. All universal rights reserved. Designated trademarks and brands are the property of their respective owners. Use of this Web site constitutes acceptance of our legal disclaimer.
|
|---|